Introduction
Cone‑beam computed tomography (CBCT) is a compact imaging system that rotates a cone‑shaped X‑ray beam around the patient’s head, capturing 150–200 high‑resolution 2‑D images in 5–40 seconds. These images are reconstructed into a true three‑dimensional volume, allowing clinicians to view teeth, bone, nerves and soft‑tissue structures from any angle without the super‑imposition seen on traditional 2‑D radiographs. Over the past two decades, advances in low‑dose protocols, high‑resolution detectors and user‑friendly software have made office‑based CBCT faster, safer and more affordable. As a result, many dental practices now consider CBCT the "gold standard" for implant planning, orthodontics, endodontics and TMJ assessment, and it is poised to become a routine diagnostic tool in everyday dental care.
Understanding CBCT: Definition and Clinical Uses
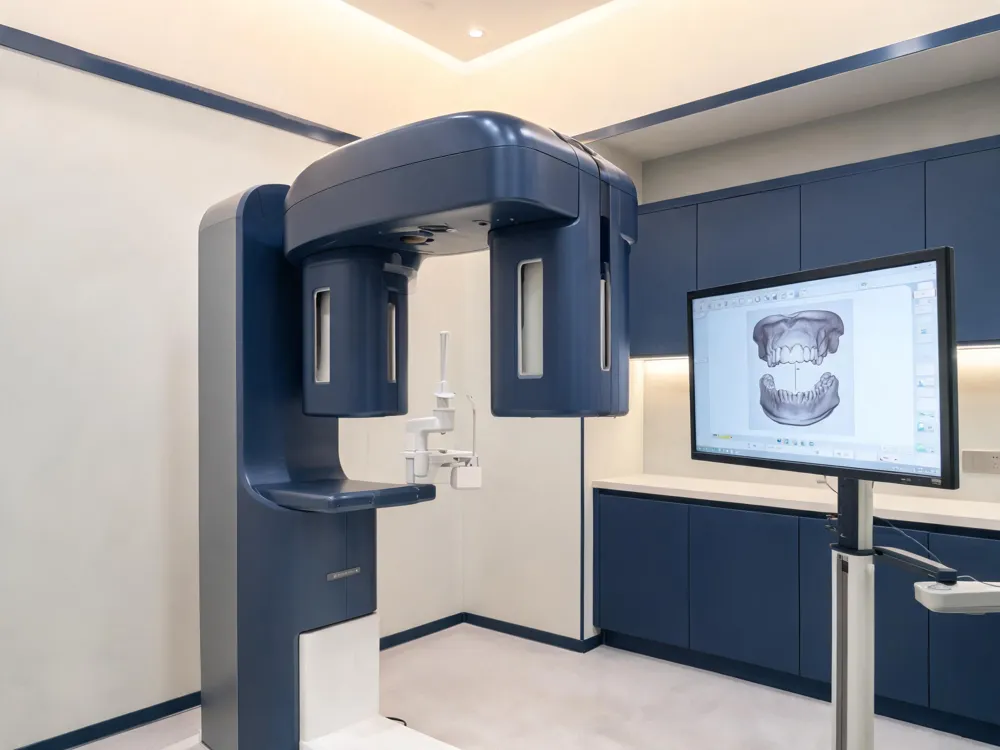 What is CBCT, and how is it used in dentistry?
CBCT, or Cone Beam Computed Tomography, is a specialized dental X‑ray technology that captures a single volumetric scan with a cone‑shaped beam rotating 180‑360°. It produces high‑resolution three‑dimensional images of teeth, bone, soft tissues, and nerve pathways, offering far more detail than conventional 2‑D radiographs while delivering a radiation dose lower than medical CT. In dental practice CBCT is employed when standard X‑rays are insufficient, supporting precise treatment planning for implant placement, surgical removal of impacted teeth, TMJ assessment, sinus evaluation, detection of jaw tumors, and orthodontic analysis. Its ability to visualize bone height, density, and proximity to vital structures enhances safety and accuracy across multiple specialties.
What is CBCT, and how is it used in dentistry?
CBCT, or Cone Beam Computed Tomography, is a specialized dental X‑ray technology that captures a single volumetric scan with a cone‑shaped beam rotating 180‑360°. It produces high‑resolution three‑dimensional images of teeth, bone, soft tissues, and nerve pathways, offering far more detail than conventional 2‑D radiographs while delivering a radiation dose lower than medical CT. In dental practice CBCT is employed when standard X‑rays are insufficient, supporting precise treatment planning for implant placement, surgical removal of impacted teeth, TMJ assessment, sinus evaluation, detection of jaw tumors, and orthodontic analysis. Its ability to visualize bone height, density, and proximity to vital structures enhances safety and accuracy across multiple specialties.
What are the basic principles and history of CBCT in dentistry? CBCT works by rotating a cone‑shaped X‑ray source and flat‑panel detector around the patient, acquiring 150–200 (or more) 2‑D images that are reconstructed into a 3‑D volume using CT algorithms such as the Feldkamp‑Davis‑Kress method. The technology traces back to the late 1990s when Yoshinori Arai’s team introduced the first dental prototype, the 3D Accuitomo. Early 2000s saw rapid commercialization (e.g., NewTom, i‑CAT), bringing faster scan times, sub‑millimeter voxel resolution, and lower radiation doses. Today, CBCT is regarded as the gold‑standard for oral and maxillofacial imaging, with ongoing advances in ultra‑low‑dose protocols, adaptive filters, and AI‑driven analysis that further improve diagnostic confidence and patient safety.
Key Dental Specialties Leveraging CBCT
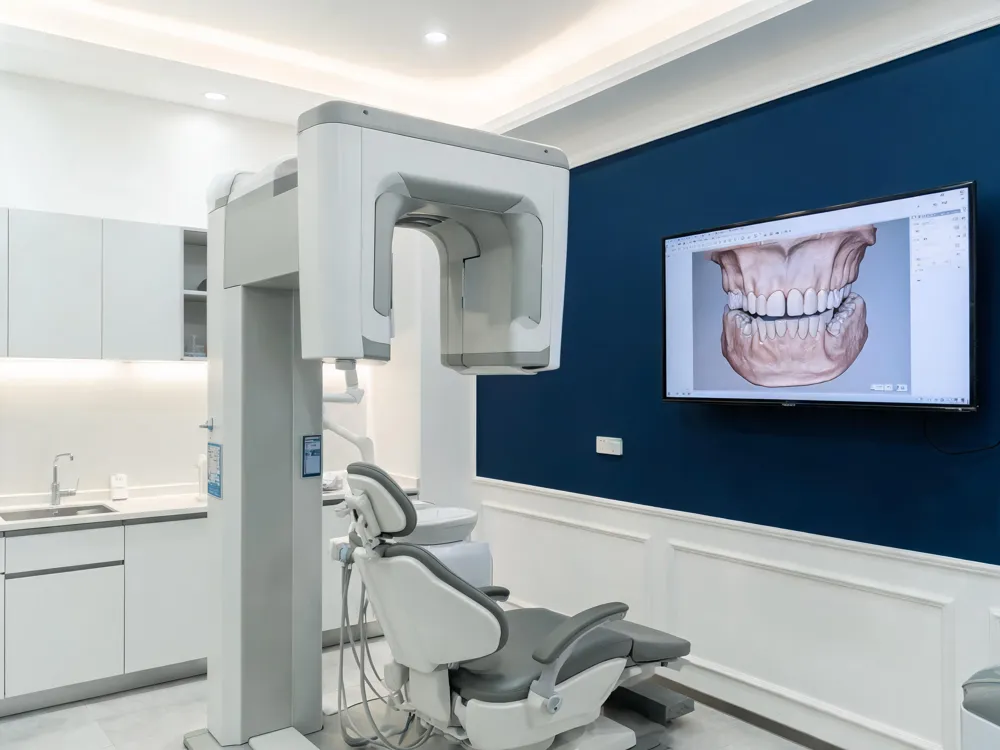 CBCT imaging delivers the greatest benefit to oral and maxillofacial surgery, where three‑dimensional views enable precise measurement of bone volume, nerve pathways, and fracture lines that 2‑D radiographs cannot reveal. Implantology also relies heavily on CBCT; the technology provides accurate assessments of bone height, width, and density, allowing virtual implant planning and the creation of computer‑guided surgical guides that reduce intra‑operative surprises. Endodontics gains from CBCT’s ability to detect periapical lesions, root fractures, and complex canal anatomy, improving diagnostic confidence and treatment outcomes. Orthodontics uses CBCT to evaluate impacted teeth, craniofacial growth, and airway dimensions, facilitating accurate appliance design and treatment monitoring. Across these specialties, CBCT’s low‑dose, high‑resolution 3‑D imaging—combined with customizable fields of view and compliance with ALARA principles—optimizes safety while delivering the detailed anatomical information essential for modern, patient‑centered dental care.
CBCT imaging delivers the greatest benefit to oral and maxillofacial surgery, where three‑dimensional views enable precise measurement of bone volume, nerve pathways, and fracture lines that 2‑D radiographs cannot reveal. Implantology also relies heavily on CBCT; the technology provides accurate assessments of bone height, width, and density, allowing virtual implant planning and the creation of computer‑guided surgical guides that reduce intra‑operative surprises. Endodontics gains from CBCT’s ability to detect periapical lesions, root fractures, and complex canal anatomy, improving diagnostic confidence and treatment outcomes. Orthodontics uses CBCT to evaluate impacted teeth, craniofacial growth, and airway dimensions, facilitating accurate appliance design and treatment monitoring. Across these specialties, CBCT’s low‑dose, high‑resolution 3‑D imaging—combined with customizable fields of view and compliance with ALARA principles—optimizes safety while delivering the detailed anatomical information essential for modern, patient‑centered dental care.
CBCT vs. Traditional Imaging
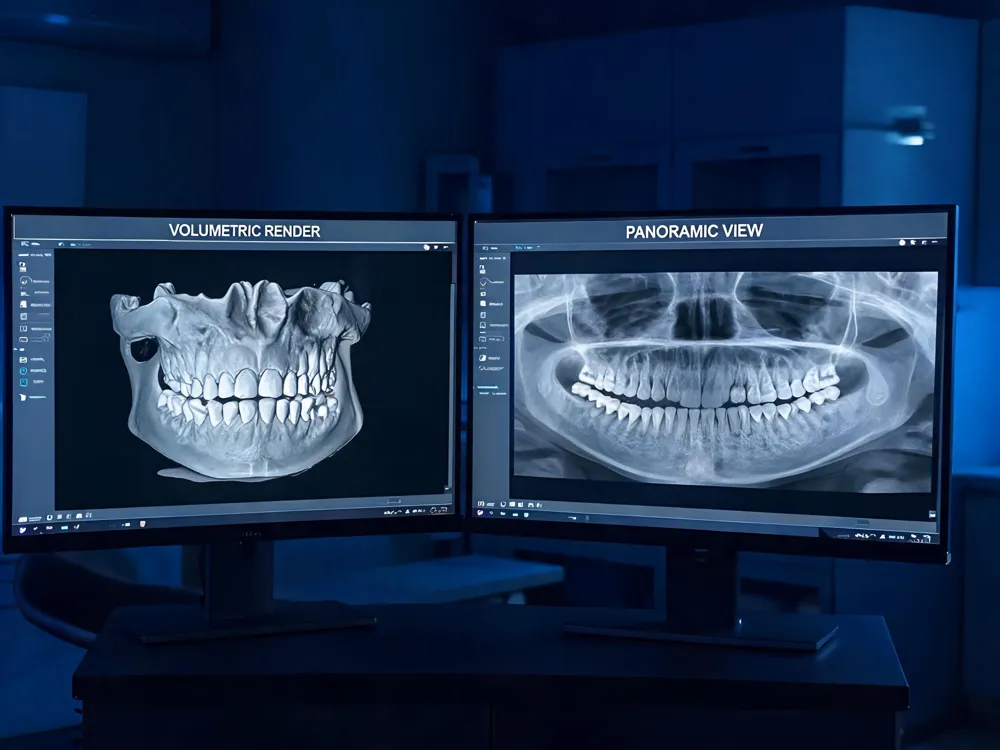 Cone beam computed tomography (CBCT) and orthopantomogram (OPG) serve distinct diagnostic purposes. CBCT captures a 3‑D volumetric dataset by rotating a cone‑shaped X‑ray beam around the patient, producing isotropic sub‑millimeter voxels (0.09‑0.4 mm) that reveal bone architecture, nerve pathways, sinus anatomy, and soft‑tissue detail from any viewing angle. This high‑resolution, distortion‑free imaging is essential for implant planning, complex orthodontic cases, TMJ assessment, and surgical navigation. OPG, by contrast, provides a single 2‑D panoramic image of the entire dentition in seconds. It is ideal for routine check‑ups, evaluating wisdom teeth, and screening for gross pathologies, offering lower cost and reduced radiation but limited depth perception and magnification.
Cone beam computed tomography (CBCT) and orthopantomogram (OPG) serve distinct diagnostic purposes. CBCT captures a 3‑D volumetric dataset by rotating a cone‑shaped X‑ray beam around the patient, producing isotropic sub‑millimeter voxels (0.09‑0.4 mm) that reveal bone architecture, nerve pathways, sinus anatomy, and soft‑tissue detail from any viewing angle. This high‑resolution, distortion‑free imaging is essential for implant planning, complex orthodontic cases, TMJ assessment, and surgical navigation. OPG, by contrast, provides a single 2‑D panoramic image of the entire dentition in seconds. It is ideal for routine check‑ups, evaluating wisdom teeth, and screening for gross pathologies, offering lower cost and reduced radiation but limited depth perception and magnification.
Radiation exposure reflects these differences. A typical dental CBCT scan delivers 19‑1,073 µSv, depending on field of view, voxel size, and protocol, whereas an OPG ranges from 5‑25 µSv. Although CBCT doses exceed panoramic images by several‑fold, they remain far below those of conventional medical CT. Clinicians follow ALARA/ALADA principles, prescribing CBCT only when the diagnostic benefit outweighs the modest increase in radiation, especially for pediatric patients.
Practical Considerations: Cost, Insurance, and Safety
 CBCT scans are increasingly routine in modern dental offices, but patients often wonder about cost, coverage, and safety during pregnancy. The typical price for a dental CBCT in the United States ranges from $100 to $500 per scan, depending on the field of view, scan complexity, and geographic location. Many practices offer financing or payment plans to make this advanced imaging affordable.
CBCT scans are increasingly routine in modern dental offices, but patients often wonder about cost, coverage, and safety during pregnancy. The typical price for a dental CBCT in the United States ranges from $100 to $500 per scan, depending on the field of view, scan complexity, and geographic location. Many practices offer financing or payment plans to make this advanced imaging affordable.
Insurance coverage varies. Most dental insurers, including Delta Dental as of 2024, will reimburse CBCT when it is medically necessary—such as for implant planning, surgical extractions, or evaluation of pathology—but routine use for simple restorations is usually excluded. Pre‑authorization and documentation of clinical justification are often required, and some plans may bill under medical codes if the scan meets medical necessity criteria.
Pregnancy safety: Although CBCT uses ionizing radiation, the fetal dose is extremely low (approximately 0.009–7.97 µSv), far below natural background exposure. The consensus is to avoid CBCT during the first trimester unless the diagnostic benefit outweighs the minimal risk. When essential, lead shielding and low‑dose protocols are employed, and the decision should be made in consultation with the patient’s obstetrician.
Integrating CBCT into Clinical Workflow
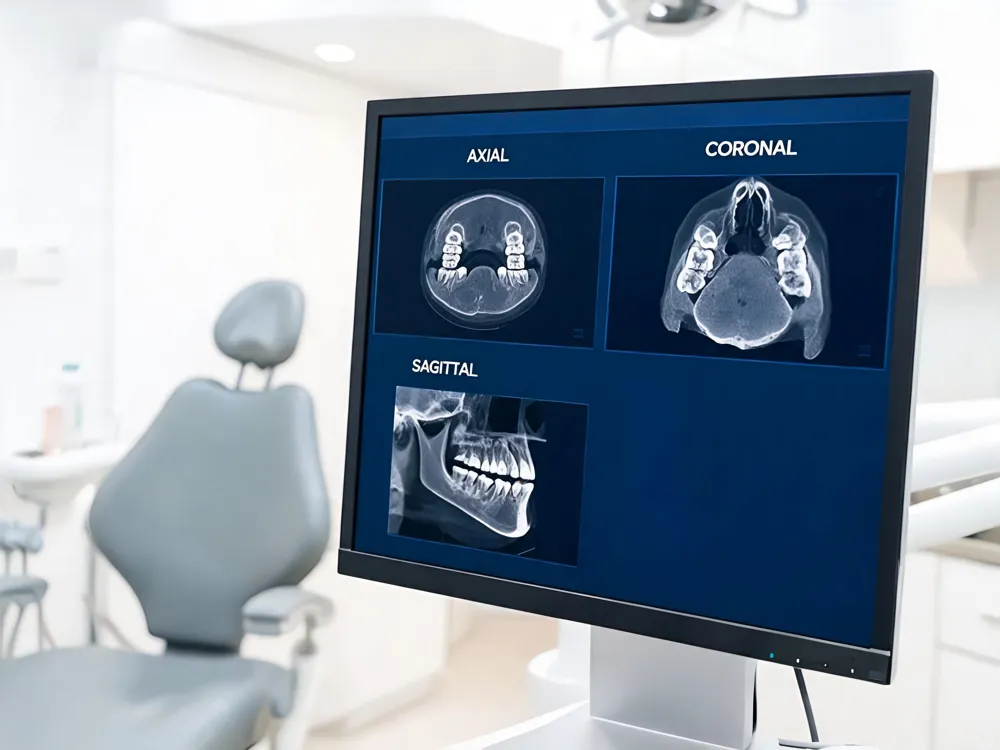 Cone‑beam computed tomography (CBCT) has become the "gold standard oral imaging with CBCT" for three‑dimensional imaging of the oral and maxillofacial region, and its systematic adoption in a dental office begins with clear interpretation basics. A practitioner starts by reviewing axial, coronal and sagittal slices to evaluate bone density, tooth morphology, and critical structures such as the inferior alveolar nerve, while also noting incidental findings like sinus pathology or airway obstruction. This 3‑D data is then applied to implant planning, orthodontic assessment, endodontic case analysis and image‑guided surgery, improving diagnostic accuracy and treatment outcomes.
Cone‑beam computed tomography (CBCT) has become the "gold standard oral imaging with CBCT" for three‑dimensional imaging of the oral and maxillofacial region, and its systematic adoption in a dental office begins with clear interpretation basics. A practitioner starts by reviewing axial, coronal and sagittal slices to evaluate bone density, tooth morphology, and critical structures such as the inferior alveolar nerve, while also noting incidental findings like sinus pathology or airway obstruction. This 3‑D data is then applied to implant planning, orthodontic assessment, endodontic case analysis and image‑guided surgery, improving diagnostic accuracy and treatment outcomes.
To ensure reliable use, staff must complete dedicated CBCT training that covers device‑specific software, patient positioning, protocol selection, and adherence to the ALARA/ALADA radiation‑safety principles. Professional workshops—such as the CB110 and CB210 courses—provide hands‑on case review and certification, while practice protocols should define when a CBCT is justified, how to select the smallest appropriate field of view, and how to document informed consent.
Regulatory compliance is essential. The FDA, ADA and European SEDENTEXCT guidelines require justification of each scan, dose‑optimization, and proper record‑keeping. Practices should maintain up‑to‑date training files, follow dose‑reduction strategies (e.g., low‑dose protocols), and retain DICOM images in a secure, HIPAA‑compliant system. By integrating these interpretation, training and regulatory steps, a dental office can safely and efficiently employ CBCT to enhance patient care.
Beyond Imaging: ROI, Patient Communication, and Future Trends
 Investing in an in‑office CBCT unit can quickly become a financial advantage. A typical practice that mixes panoramic radiographs with a few implant, third‑molar, and endodontic scans can generate several thousand dollars of monthly revenue, and the additional case‑acceptance rates for high‑value procedures—often 70‑80 %—translate into a strong return on investment within the first year.
Investing in an in‑office CBCT unit can quickly become a financial advantage. A typical practice that mixes panoramic radiographs with a few implant, third‑molar, and endodontic scans can generate several thousand dollars of monthly revenue, and the additional case‑acceptance rates for high‑value procedures—often 70‑80 %—translate into a strong return on investment within the first year.
Patient education is dramatically enhanced when we can show a three‑dimensional model of the patient’s own anatomy. 3‑D visualizations turn abstract findings into clear, interactive images that patients can explore, boosting understanding, trust, and consent rates.
Artificial‑intelligence platforms now read CBCT volumes in real time, automatically highlighting bone loss, periapical lesions, and critical anatomical landmarks. This AI‑driven workflow reduces diagnostic fatigue, standardizes measurements across the team, and shortens treatment‑planning time, allowing clinicians to move from diagnosis to a definitive plan in a single appointment.
Low‑dose and ultra‑low‑dose protocols, guided by the ALARA/ALADA principles, keep patient exposure well below that of conventional medical CT—often 87 % lower than standard CBCT scanners—while preserving the image quality needed for implant planning, orthodontic analysis, and endodontic assessment. By selecting the smallest appropriate field of view, adjusting tube current and voltage, and using modern iterative‑reconstruction software, practices can meet safety standards and reassure patients about radiation risks.
Conclusion
In summary, cone‑beam computed tomography delivers the gold‑standard 3‑D imaging needed for accurate diagnosis, precise treatment planning, and safer outcomes across implantology, orthodontics, endodontics, oral surgery, and TMJ assessment. The technology’s low‑dose protocols, rapid scan times, and seamless integration with digital workflows enhance patient education, reduce chair‑time, and support evidence‑based decisions while adhering to ALARA principles. Southern Boulevard Dental in Rio Rancho, New Mexico, invites you to experience the benefits of in‑office CBCT. Schedule a consultation today to see how our advanced imaging, combined with a caring, family‑focused team, can personalize your treatment plan and improve your oral health.
